March 9, 2011 — The United States relies heavily on foreign physicians to supply health care to Americans, especially when it comes to providing primary care. Foreign physicians are also concentrated in underserved communities. For several decades, there have not been enough U.S. medical school graduates to fill the slots available in domestic residency programs, and those that are left over go to international medical graduates, or IMGs. In 2010, for example, more than 20 percent of graduates who were matched to first-year residency positions had graduated from foreign schools.
With an intensification of the U.S. doctor shortage looming, one suggested stopgap is to increase the U.S.’s reliance on foreign physicians. The proposal takes two basic forms. Some advocate for “passive recruitment” — a policy under which the number of funded slots at U.S. residency programs would be increased and those additional slots filled, at least in the short-term, with graduates of foreign medical schools. This increase should come hand-in-hand with the relaxation or elimination of current restrictions and bureaucratic regulations on foreign physicians, proponents argue, thereby making it easier for foreign physicians to stay and practice in the U.S. after they have completed their residency programs here.
A more radical proposal, known as “active recruitment,” is to lift altogether the current requirement that any foreign physician who wishes to obtain a license to practice medicine in the U.S. complete a residency program here. Several other countries, including Canada and the United Kingdom, engage in active recruitment to address their own physician shortages, or have in the past.
The proposals raise questions about how best to deal with the fact that standards for both medical school education and residency training vary from country to country; the fact that relaxations on limitations of IMGs would not increase the number of doctors in the pipeline if the existing cap on the number of funded residencies weren’t lifted; or the fact that attracting foreign doctors to the U.S. would exacerbate doctor shortages in other countries.
The proposals also have to contend with another frequently observed phenomenon: the tendency of solutions that are touted as “temporary” to harden into permanent arrangements. Would either passive or active recruitment have the perverse effect of stymieing efforts to increase the number of U.S. medical school graduates, or mean that the “zero sum” problem of shifting doctors from other countries to the U.S. would be ignored over the long term?
Active recruitment
Currently, in order to obtain a license to practice medicine in the U.S., all foreign medical school graduates are required to complete a medical residency program of at least three years in the U.S. But Richard Cooper, former dean of the Medical College of Wisconsin, suggested that, in order to alleviate the physician shortage here, the U.S. should pursue a strategy of active recruitment of physicians abroad, in which the requirement to complete residency training in the U.S. is waived for qualified doctors.
“The United States is the only country in the world that requires foreign medical students to do their residencies here before they can practice,” he said.
According to Ivy Lynn Bourgeault, professor of health sciences at the University of Ottawa, Canada currently allows foreign doctors to practice through two channels. One is similar to the model used in the U.S., where IMGs come to do residency training here and can thereafter be certified to practice. The other involves active recruitment by understaffed hospitals, health centers or communities of foreign physicians, who are then granted a provisional license.
The United Kingdom aggressively pursued a similar policy in the past, recruiting extensively from other Commonwealth countries like India and South Africa.
“It would be fast, almost immediate, and it would be cheap, too,” Cooper said.
Opponents, such as Edward Salsberg, director of the National Center for Workforce Analysis, which is housed in the Department of Health and Human Services, argue that the requirement that foreign graduates complete residency training in the U.S. is the foremost safeguard for ensuring quality of care.
“We have some of the highest standards in the world, and it’s in everybody’s interest that they be maintained,” he said.
But Daniel Purdom, a family practitioner in Kansas City, argued that requiring that IMGs complete medical residency programs in the U.S. is not the only way to ensure quality. One option, he said, would be for the U.S. to impose qualification requirements on individual physicians, based on competency and language tests, like Canada does (see sidebar).
Salsberg argued that this wouldn’t go far enough to ensure quality.
“In general, we don’t think that just passing a test is going to [provide] sufficient confidence of the qualifications of the individual physicians,” he said.
Another way to assure physician quality, Purdom said, would be to allow a U.S. organization — most likely the Accreditation Council for Graduate Medical Education, which is responsible for certifying U.S. programs — to certify residency programs in other countries.
“That certainly would give more comfort,” Salsberg agreed. “That would have to be looked at.”
But Salsberg pointed out that the requirements of residency programs in other countries vary substantially. Some countries from which the U.S. currently accepts physicians — particularly African countries — don’t even require residency training, he said, and others in Europe, Asia and South America require only two years.
“It isn’t necessarily in the interest of these programs to change their requirements to meet U.S. standards,” he said, which means that, before approving other programs, the U.S. would have to determine which ones come close enough to U.S. standards to qualify for certification.
Salsberg admitted that there are likely several foreign residency programs suitable for evalution by U.S. standards, particularly in Europe, but narrowing the pool to those programs could significantly limit the numbers of new physicians that could be recruited to the U.S. through this proposal, he said.
Purdom argued that every state is already responsible for setting the standards a physician must meet to obtain a license to practice in that state.
Additionally, residency programs in many states, such as New York, already have recruitment in place programs to attract foreign medical graduates. Those programs could theoretically serve as models for hospitals and health centers that want to employ foreign physicians who have already completed residency training abroad.
Salsberg, who is opposed to relying more heavily on foreign doctors, said that he didn’t see recruitment being part of U.S. policy anytime soon.
“We haven’t even gotten to the point where we’re accrediting foreign medical schools yet,” he said. Last year, the Educational Commission for Foreign Medical Graduates (ECFMG) announced that it will be 2023 before it requires all foreign physicians to graduate from a medical school that has been accredited by the Liaison Committee on Medical Education.
Passive recruitment
Much of the effort to increase the U.S. physician supply has centered on increasing the number of medical residency positions — or graduate medical education (GME) slots — that are partially funded by the government, primarily through Medicare. The number was capped at about 100,000 in 1997.
The Association of American Medical Colleges and the American Medical Association argue that the U.S. will not be able to meet its need for more physicians if the cap remains in place.
But if the cap were lifted immediately, residency programs would not find large numbers of U.S. medical school graduates ready to fill newly-created spots. Nearly all graduates of domestic medical schools are already “matched” into residency programs. Thus, unless U.S. medical school enrollments were greatly expanded — as many have urged, so far unsuccessfully — an increase in the residency cap would effectively result in residency programs turning to IMGs to fill most of the new slots.
Historically, some justification for limiting U.S. reliance on foreign medical graduates has been based on questioning the quality of those graduates.
Elizabeth Garvish, an immigration attorney based in Atlanta, argued that foreign medical graduates provide at least the same level of care as U.S. trained physicians, and already have to pass several tests before they can even apply to a U.S. residency program. Those tests include an examination of clinical knowledge, a hands-on clinical skills exam, and an English-language exam.
A study by researchers at the Foundation for Advancement of International Medical Education and Research, published last year, reinforced that argument. The study found that foreign graduates perform as well as U.S. graduates, and actually perform better than American nationals who attended medical school abroad and then return to do their residency training in the U.S.
Currently, there is a high level of competition for IMGs who seek a residency slot in the U.S. Though 93 percent of U.S. medical school graduates were matched last year to first-year residency positions in the U.S., only 40 percent of IMGs were. What would happen if significantly more residency positions were created and then filled by IMGs?
Salsberg acknowledged that there would be a short-term reduction in the competitiveness of U.S. residency slots for graduates of foreign medical schools if the cap on residencies were lifted in the near future, and added: “That’s just another reason why we have to get our production up domestically.”
Brain drain
Even if the quality of foreign physicians were ensured, Kate Tulenko, director of Intrahealth, a public health organization, argued that, when viewed internationally, physician migration is inherently a zero-sum equation.
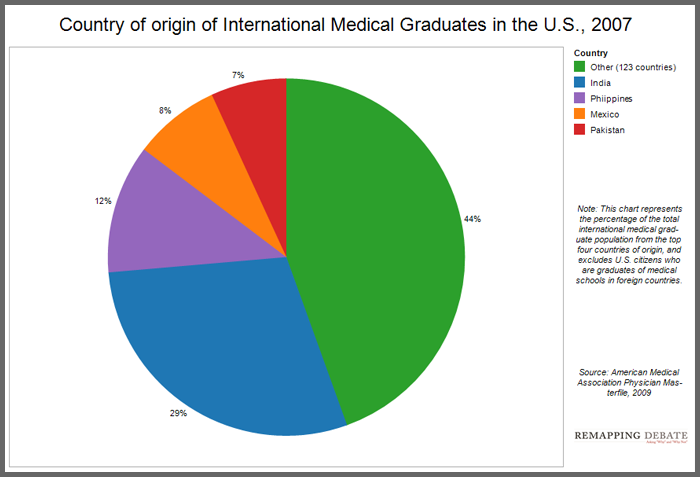
After U.S. nationals who travel abroad to attend medical school (who are still considered international medical graduates), the largest numbers of IMGs come from India, the Philippines, Pakistan, and Mexico (see chart below). Tulenko pointed out that all of these countries have physician shortages of their own, and that the World Health Organization has classified India and Pakistan as “health workforce crisis countries.”
Many of the foreign physicians who would be recruited to work in the U.S. would likely come from these same countries, Tulenko said.
“The countries that people come from are left without healthcare workers to take care of their pressing needs,” she said, adding that recruitment of physicians by wealthy countries and recruitment of nurses by the U.S. have only exacerbated the problem.
Bourgeault agreed, calling reliance on foreign physicians an “ethical gray area.” The policy of recruiting nurses from abroad has also been widely critiqued on brain drain grounds. Indeed, Salsberg pointed out that last year, the U.S. signed a “code of practice,” along with 193 other countries at the World Health Assembly, in which voluntary principles for “the ethical international recruitment of health personnel” were endorsed in order to lessen recruitment from lower income countries with “fragile health systems.”
Garvish dismissed ethics-based arguments against foreign recruitment, saying that it “may be the case” that the U.S. is depriving other countries of their health workforce, “but I don’t know if the U.S. is supposed to make sure that every country out there has enough qualified doctors to care for their people. It’s a free world, and I think the U.S. needs to deal with its own issues.”
Tulenko, however, argued that the reliance on foreign medical graduates is so unethical that the U.S. should dramatically increase medical school enrollments before adding any new residency positions.
Cooper acknowledged that, because of these ethical issues, foreign recruitment of physicians would not be a good long-term strategy, and should only be employed in the short-term as the U.S. simultaneously ramps up its education and training capacity.
Medical school enrollments have increased somewhat in recent years in an attempt to address the physician shortage, but they are relatively minor increases in relation to the projected need. In 2006, the Association of American Medical Colleges (AAMC) called for a 30 percent increase in enrollment by 2015 – or 5,000 new M.D. students annually. Between 2006 and 2010, enrollment increased by only 7.5 percent. At that rate, medical school enrollments will fall far short of the AAMC’s goal.
A dramatic increase in the number of medical schools — an increase that would allow both new and existing residency slots to be filled by U.S. medical graduates — would not be unprecedented, however. As Remapping Debate recently reported, in the 1960s and ‘70s, enrollment at U.S. medical schools more than doubled in response to projections of a physician shortage. This expansion was largely due to funding from the 1963 Health Professions Education Assistance Act, which provided grants for the construction of new facilities and the expansion of existing schools.
Additionally, Tulenko said, “There is already a surplus of qualified applicants [from the U.S], who are going to medical schools abroad, mostly in the Caribbean.”
A substitute for long-term policy?
Some worry that increasing the reliance on foreign medical graduates would distract from the pressing need to increase domestic medical school enrollment. Fitzhugh Mullan, a professor of health policy at George Washington University, has argued that, without IMGs, the U.S. would already have faced a substantial physician shortage.
The U.S.’s reliance on foreign physicians exemplifies the fact that short-term policy to address immediate needs can often end up becoming long-term policy, and even substitute for a more comprehensive approach.
When the number of residency programs in the U.S. was increased in the 1960’s and ‘70s, the number of foreign medical graduates skyrocketed, despite the large increase in domestic medical school enrollment. But medical school enrollment flattened out in the 1980s, despite calls for decreasing the reliance on foreign physicians.
According to Mullan, reliance on foreign medical school graduates was supposed to be a temporary solution, but U.S. medical school enrollments were never increased substantially past the level they reached in the early 1980s and, in effect, reliance on foreign medical graduates has became long-term policy.
Bourgeault said that further increasing U.S. reliance on foreign physicians now has the same risk.
“I think it’s a short-term ‘solution,’” she said, qualifying the word solution because she was not sure that it really solved more problems than it caused. She argued that, with the political will, a wealthy country like the U.S. should be able to train enough of its own physicians to meet its needs.