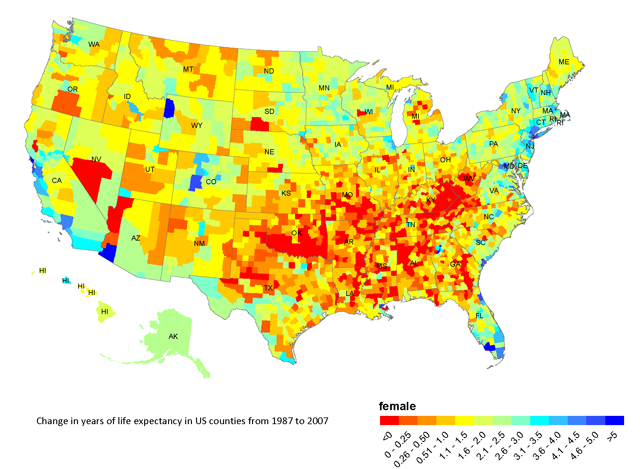
June 22, 2011 — Every generation born in the United States has lived longer than the one before, and so it has been easy to assume that the upward trend would continue. But while life expectancy in the country as a whole has continued to rise steadily for the last twenty years, a new study shows that life expectancy for women has actually declined during this period in 313 U.S. counties, most in the Southeast, the Southern Midwest, and Appalachia. Life expectancy for men, by contrast, only declined in six counties (although the study did find that men in these same areas tended to have worse outcomes than men elsewhere). In what some experts have dubbed a public health crisis, these findings mean that children born today in many parts of the United States can expect to live shorter lives than their parents.
“We have talked about this trend as being the biggest decline in life expectancy since the Spanish flu epidemic of 1918 in the U.S.,” said Ali Mokdad, a professor of global health at the Institute for Health Metrics and Evaluation (IHME) at the University of Washington, which issued the report. “There is no perfect analogue, though, because what we are seeing is not the result of an epidemic in the traditional sense.”
Using data culled from death certificates by the National Center for Health Statistics, an arm of the Centers for Disease Control (CDC), researchers at the IHME drilled down to the county level to track life expectancy from 1987 to 2007.
In addition to the gender disparities, the regional variations are striking: while life expectancy increased in the North with few exceptions, huge swathes of the South saw decreases for women, in some cases by as much as nearly two years. Decreases were particularly concentrated in Alabama, Kentucky, Mississippi, Missouri, Oklahoma, Tennessee, and West Virginia.
Mokdad speculated that increases in the prevalence of major risk factors for chronic diseases — especially obesity and smoking among women — were probable, though not definitive, causes of lower life expectancy.
Remapping Debate spoke with several county and state public health officials in areas where life expectancy decreased, anticipating that we would get a clearer picture of what was happening on the local level. While some were not surprised to hear about the IHME’s findings, others expressed bewilderment.
“That is just so surprising,” said Gino Solla, director of the Ector County Health Department, in eastern Texas, where life expectancy for women decreased by more than seven months between 1987 and 2007. “I could offer you an explanation, but I’d just be shooting in the dark.”
Appalachia
Patrice Beverly is the Health Education Coordinator for Pike County, Kentucky, on the eastern tip of the state bordering Virginia and West Virginia. Life expectancy for women decreased in nearly all of this region. But Pike County is one of only two counties in the country in which life expectancy decreased for both men and women.
“For men, that makes more sense, because so many men work in the coal mines,” Beverly said, adding that a larger proportion of men are employed in mining than in the past for lack of other opportunities. “But I don’t know about the women. The only trend that I can think of is possibly that women have gone back to work, which adds the stress of keeping up a job to keeping up a family.”
Beverly also said that there’s a large problem with health care access in Pike County. “A lot of families live kind of off the road,” she said, “and it’s hard to get in there to check on people.”
But she said that she personally attributes the health problem to cultural trends more than economic ones. “We tried for a long time to get adults to stop smoking, eat better, exercise, but I’ve realized that at a certain point, it becomes very hard to change people in their life’s journey,” she said.
Instead, the public health department in Pike County has been focusing on young people, she said, by going into schools to educate children on the benefits of healthy habits and the dangers of unhealthy ones.
Nearby in McDowell County, West Virginia, Public Health Department administrator Jesse Rose echoed that sentiment. “We try to help everybody we can,” he said, “but mindset has a lot to do with it, and that’s hard to change.”
McDowell has one of the lowest life expectancies, for both men and women, in the country. Life expectancy has not changed at all for men since 1987, and has decreased for women by nearly 10 months.
“It’s the women I don’t understand,” he said. “It seems like when we have clinics, it’s mostly women who come. I’m puzzled. I know we weren’t doing so great compared with the rest of the country, but I thought we would be doing better then we were.”
Oklahoma
Judith Duncan, the director of physical activity and nutrition in the Oklahoma State Department of Public Health, was similarly puzzled when she heard that life expectancy had either declined or remained level in most counties in Oklahoma. In fact, Oklahoma is the only state in the country in which life expectancy for women decreased at the state level, from 78.5 years in 1987 to 77.9 in 2007. For men, it increased slightly during the same period, by a little more than one year.
“If I had the answer to why this is happening I would be a wealthy woman,” Duncan said.
Much of southern Oklahoma is rural, and the poverty rate in those counties is well above the national figures. Duncan also said that there are a relatively small number of primary care physicians in the state, which caused problems with access to care, especially in rural areas.
Sally Carter, another state public health official who concentrates primarily on tobacco use, said that smoking rates were particularly high in that part of the state, especially among women. In recent years, the state has been concentrating increasingly on that issue, starting a “quit line” that people who are quitting smoking can call for support and issuing free nicotine patches and gum to some residents.
But Duncan emphasized that there is only so much that Public Health Departments can do in Oklahoma, or anywhere else in the country. “Funding is obviously an issue, not just here but everywhere,” she said. “But there are some things we could do quickly that don’t cost a lot of money. There are policies that could be made at the state and federal level that would have enormous benefits at low costs.”
In Oklahoma, she said, there is no mandated requirement for health education classes in high school. She also mentioned banning smoking in restaurants and public places and setting aside property for community gardens to increase access to food.
Duncan acknowledged, however, that recent budget cuts have made it harder to do her work by reducing the staff available for the programs the Department runs. She said that, if the funding were available, she would be eager to invest in infrastructure such as sidewalks and green space to make it easier for residents to exercise. She would also like to introduce initiatives to increase the amount of fruits and vegetables available in grocery stores, and to run “counter-marketing” campaigns to highlight the dangers of tobacco use.
But those initiatives will have to wait. “I don’t see our budget increasing anytime soon,” Duncan said. “We’re trying to do more with less, and think of innovative solutions. The problem is, when you’re trying to create programs with long-term benefits and then funding gets cut, it takes you twice as long to recover even when your funding comes back.”
During the 2010 fiscal year, the Oklahoma State Department of Health saw its funding cut by 7.5 percent, which has not been restored in the current budget. In 2010, the cuts prompted State Commissioner of Health Terry Kline to tell state legislators that, “Oklahoma is about to become the public health joke of the country.”
The Mississippi delta
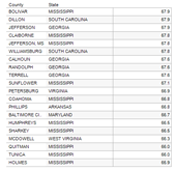
The life expectancy in Mississippi was the lowest in the country in 2007, at 77.9 years for women and 70.9 years for men, trailing the national figures by several years in both cases. And in one fifth of Mississippi counties, things are getting worse.
In Sunflower County, a county of fewer than 30,000 people near the Mississippi River in the northeastern part of the state, life expectancy for women decreased more significantly than virtually anywhere else in the country, from 75.5 years in 1987 to 73.6 years in 2007. That number gives Sunflower the dubious honor of having the second lowest life expectancy for women of any county in the country; first place goes to nearby Holmes County, where life expectancy for women decreased by nearly a year (to 73.5 years) in the same period.
Alfio Rausa, the district health officer for 18 counties in the Mississippi delta including Sunflower and Holmes, was not surprised that Sunflower fared so poorly; if anything, he was surprised that many of the surrounding counties had improved.
“Things in the Delta have only gotten worse in the last 20 years,” Rausa said. “There are fewer job opportunities, fewer programs, more unemployment, more poverty.”
Sunflower is notable for having an exceptionally high obesity rate — 41 percent of adults in the county are obese, according to the CDC — and 46 percent of children in Sunflower live in poverty. The teen pregnancy rate is twice the national average, according to the CDC, and 65 percent of children live in a single-parent household.
Rausa noted other factors that are less commented upon but which he said were also contributing to poor health in the region.
“These counties are so small, that they can’t support a supermarket,” he said. “If you live in the northern part of the county, you might have to drive 90 minutes to get to Indianola,” the county seat and nearest large town. “There’s a Wal-Mart there that has decent produce.”
Additionally, Rausa said that he had noticed more people living in very poor conditions, especially in rental apartments. “There’s no state law in Mississippi that says that in order for a property to be rentable, it has to meet certain health criteria,” he said. “So you see people living in places with dirty water, asbestos, infestations.”
Rausa said that the public health department has been “flat-funded” for the last several years, despite an increase in demand for services. The CDC recently issued a grant to the public health department in the delta region for a demonstration project to prevent heart disease, stroke and other chronic diseases, and some projects aimed at increasing access to healthy food and educating children about healthy habits began this year, Rausa said.
But, overall, he doesn’t see much changing until the socioeconomic risk factors are addressed. “I don’t think people in other parts of the country can imagine how people are living down here,” Rausa said. “We’ve been left behind.”
Why is this happening?
Though researchers have long speculated about the causes of regional disparities in health outcomes, many are hard-pressed to explain an absolute decline in life expectancy in some places, because doing so requires determining which factors have gotten worse in the last two decades.
Mokdad and his colleagues and the IHME prioritize behavioral factors, such as smoking, exercise and eating habits. CDC data shows that none of the states which experienced declines in life expectancy from 1987 to 2007 had obesity rates of more than 15 percent of the population as of 1990; by 2009, however, the obesity rate was more than 30 percent in all of them, and had not risen as fast in any other states.
That could partially explain why the decline was so much more pronounced for women than for men, because women typically have higher obesity rates and also suffer greater health consequences from obesity than men do. Others have pointed out that smoking trends have not decreased as quickly for women as they have for men, and that the consequences of beginning smoking in the mid-part of the century can explain more of the disparity.
Regional disparities in life expectancy have often been attributed to differences in socioeconomic factors like family income, but IHME researchers searched for a correlation along these lines and found that only about 10 percent of the decline could be attributed to change in income or demographics.
David Kindig, an emeritus professor of population health sciences at the University of Wisconsin’s Population Health Institute who said the study’s “shocking” findings on life expectancy should be a “call to action,” cautioned that social factors should not be dismissed as a cause.
“All of the evidence we have shows that the social determinants of health are just as important over time as medical care and behaviors,” he said. Kindig noted that he and his colleagues at the University of Wisconsin had found a correlation over time between life expectancy and child poverty. He noted, however, that it is very difficult to isolate and study individual factors. “We know there is this huge web of causality,” he said. “All of these factors are connected.”
Peter Muennig, an associate professor of health policy at Columbia University’s Mailman School of Public Health, agreed that more research needed to be done to tease out what impact social and economic factors have played.
It’s very difficult to identify precisely what percentage of the decline is properly attributed to any one factor, he said, “but we know that income plays a very large role in determining adult health outcomes.” Muennig added that some indicators of socioeconomic change may not be revealed by a measure that looks only at income, including key indicators like access to health care, investments in public health, and safety net programs. He used Medicaid, which requires matching state funding as a condition for participation, as an example: “Some states and counties do not have enough money to match the funding they get from the federal government for Medicaid,” he said. “So they don’t do it, which makes it harder for people in rural areas to get care.”
And because many of the risk factors that have increased are also associated with lower incomes and educational attainment, it becomes difficult to know whether it will be more effective, in the long run, to target the risk factors themselves or to address the underlying issues, he said.
Who’s in charge here?
“When you look at mortality rates, you usually look at nations and states, and over time they almost always get better, just at slower rates,” Kindig added. “When you drill down and see these types of trends at the local level, though, that’s surprising and important.”
Bob Anderson, the chief of the mortality statistics branch of the National Center for Health Statistics at the CDC, said that the first step is to go into the communities and figure out what’s causing the decline.
“To try to come at this from a programmatic or policy perspective, it’s not enough to know that it’s happening. We really need to figure out why.” Anderson said that his staff was “itching” to do that analysis, but that the department was “barely staying on top of data production as it is.”
Anderson also said that states vary tremendously in the resources they deploy to collect data and develop evidenced-based local solutions.
Kindig agreed, and added that one of the major barriers to improving public health has been a lack of accountability, both at the local and national level. “The problem is that it’s nobody’s responsibility. There are so many sectors involved in this that nobody is really in charge.”
A national problem
Kindig emphasized that it was critical to think of the disparities as a national problem, because localized trends in public health can have a “multiplier effect,” passing — and worsening — from one generation to the next, and even spreading into other regions if left unchecked.
“Changing these trends is very much in the social and public interest,” he said. “We can’t just assume that everybody is going to get better eventually if we continue down the same path.”
“If we tripled our investment in public health, and did it in a smart way, we would almost certainly get that money back in savings in the long run because fewer people would be going to the hospital for heart attacks and strokes and cancer and diabetes.”
But the increasing political pressure to cap health care costs, he added, creates a vicious cycle. As more money is spent on treatment, the temptation is to spend less money on public health initiatives that are aimed at prevention. With fewer funds available to increase access in underserved areas, improve environmental conditions, and enhance health awareness, even more money will have to be spent on treatment, ultimately squeezing public health budgets even further.
Mokdad of the IMHE pointed out that there are also many localities have improved significantly over time, including all the boroughs of New York City. Manhattan, for example, has seen a huge jump in life expectancy over the last twenty years, from 76.6 years to 83.7 years for women and from 65.8 years to 78.7 years for men. Researchers credit the changes to the increase in income, the decrease in crime, the development of better drugs to treat HIV/AIDS, and policies to curb smoking and increase access to quality food.
“We shouldn’t think that we have a doomsday stamp on our heads,” he said. “This is our life expectancy, and we can change it” both at the individual level and at the societal level.
Kindig added that while Americans “have a pretty high tolerance for inequality,” the scope of regional and gender disparities should put officials into “crisis mode.”
“We’ve known about the disparities in the health care system for a long time,” he said, “but we’ve tolerated them because, on the whole, we were getting better. Until recently, we didn’t know that a lot of the country was actually getting worse.”