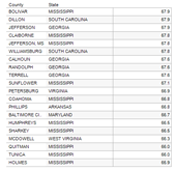
Life getting shorter for women in hundreds of U.S. counties
Peter Muennig, an associate professor of health policy at Columbia University’s Mailman School of Public Health, agreed that more research needed to be done to tease out what impact social and economic factors have played.
It’s very difficult to identify precisely what percentage of the decline is properly attributed to any one factor, he said, “but we know that income plays a very large role in determining adult health outcomes.” Muennig added that some indicators of socioeconomic change may not be revealed by a measure that looks only at income, including key indicators like access to health care, investments in public health, and safety net programs. He used Medicaid, which requires matching state funding as a condition for participation, as an example: “Some states and counties do not have enough money to match the funding they get from the federal government for Medicaid,” he said. “So they don’t do it, which makes it harder for people in rural areas to get care.”
And because many of the risk factors that have increased are also associated with lower incomes and educational attainment, it becomes difficult to know whether it will be more effective, in the long run, to target the risk factors themselves or to address the underlying issues, he said.
Who’s in charge here?
“When you look at mortality rates, you usually look at nations and states, and over time they almost always get better, just at slower rates,” Kindig added. “When you drill down and see these types of trends at the local level, though, that’s surprising and important.”
Bob Anderson, the chief of the mortality statistics branch of the National Center for Health Statistics at the CDC, said that the first step is to go into the communities and figure out what’s causing the decline.
“To try to come at this from a programmatic or policy perspective, it’s not enough to know that it’s happening. We really need to figure out why.” Anderson said that his staff was “itching” to do that analysis, but that the department was “barely staying on top of data production as it is.”
Anderson also said that states vary tremendously in the resources they deploy to collect data and develop evidenced-based local solutions.
Kindig agreed, and added that one of the major barriers to improving public health has been a lack of accountability, both at the local and national level. “The problem is that it’s nobody’s responsibility. There are so many sectors involved in this that nobody is really in charge.”
A national problem
Kindig emphasized that it was critical to think of the disparities as a national problem, because localized trends in public health can have a “multiplier effect,” passing — and worsening — from one generation to the next, and even spreading into other regions if left unchecked.
“Changing these trends is very much in the social and public interest,” he said. “We can’t just assume that everybody is going to get better eventually if we continue down the same path.”
“If we tripled our investment in public health, and did it in a smart way, we would almost certainly get that money back in savings in the long run because fewer people would be going to the hospital for heart attacks and strokes and cancer and diabetes.”
But the increasing political pressure to cap health care costs, he added, creates a vicious cycle. As more money is spent on treatment, the temptation is to spend less money on public health initiatives that are aimed at prevention. With fewer funds available to increase access in underserved areas, improve environmental conditions, and enhance health awareness, even more money will have to be spent on treatment, ultimately squeezing public health budgets even further.
Mokdad of the IMHE pointed out that there are also many localities have improved significantly over time, including all the boroughs of New York City. Manhattan, for example, has seen a huge jump in life expectancy over the last twenty years, from 76.6 years to 83.7 years for women and from 65.8 years to 78.7 years for men. Researchers credit the changes to the increase in income, the decrease in crime, the development of better drugs to treat HIV/AIDS, and policies to curb smoking and increase access to quality food.
“We shouldn’t think that we have a doomsday stamp on our heads,” he said. “This is our life expectancy, and we can change it” both at the individual level and at the societal level.
Kindig added that while Americans “have a pretty high tolerance for inequality,” the scope of regional and gender disparities should put officials into “crisis mode.”
“We’ve known about the disparities in the health care system for a long time,” he said, “but we’ve tolerated them because, on the whole, we were getting better. Until recently, we didn’t know that a lot of the country was actually getting worse.”